PROCESS-A
PROspective Cohort study Examining Self-harm and Suicide in Adolescents
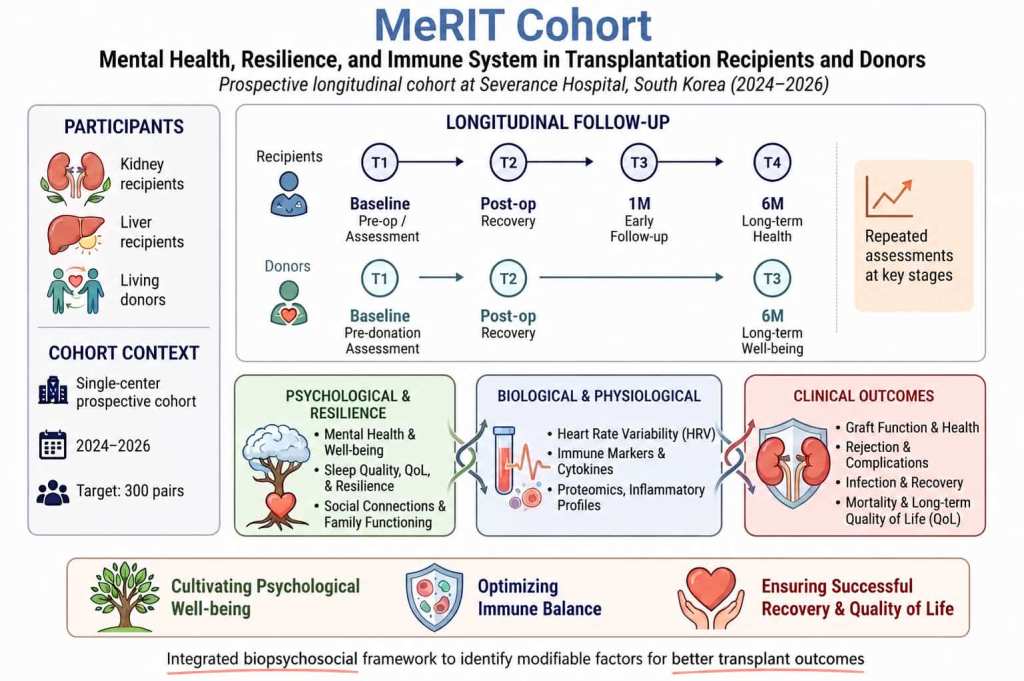
PROCESS-A (PROspective Cohort study Examining Self-harm and Suicide in Adolescents) is South Korea’s largest prospective cohort on adolescent self-harm and suicide. Anchored at Yonsei University College of Medicine and conducted in collaboration with five institutions across the greater Seoul metropolitan area, PROCESS-A follows 800 adolescents — a community control group, a non-suicidal self-injury (NSSI) group, and a suicide attempt group — over up to six years, with assessments every six months. The cohort aims to identify psychiatric, psychological, biological, and social determinants of adolescent NSSI and suicidal behavior through longitudinal observation, while simultaneously developing and validating a Korean-specific assessment tool for NSSI intent discrimination and evidence-based clinical guidelines. Ultimately, findings from the cohort will inform the development and testing of targeted intervention programs for adolescents at risk of NSSI and suicide.
Data collection spans multiple levels and modalities. Adolescents undergo structured assessments of depression, anxiety, suicidality, and self-harm behavior, complemented by validated psychometric scales across domains such as rumination and impulsivity. Caregiver mental health and parenting behaviors are assessed in parallel. Biomarker profiling encompasses inflammatory markers, stress hormones, autonomic function, and multi-modal neuroimaging including structural MRI, diffusion tensor imaging, and resting-state and task-based fMRI. These primary data are further contextualized by school environment, peer relationships, social media use, and adverse childhood experiences, with plans for future linkage to national administrative databases to enable long-term outcome ascertainment.
CC-MHS
CMERC COVID-19 Mental Health Study
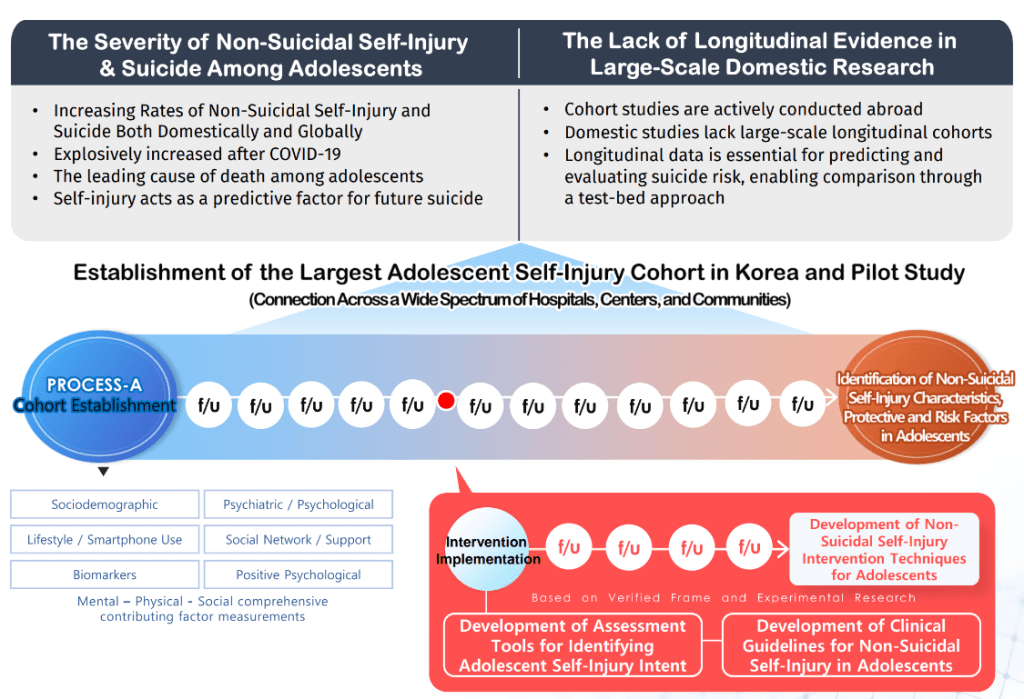
The Cardiovascular Metabolic Etiological Research Center COVID-19 Mental Health Survey (CC-MHS) represents a pioneering longitudinal initiative designed to decode the complex interplay between pre-existing health status and the psychological repercussions of a global crisis. By uniquely leveraging robust baseline data from the Cardiovascular Metabolic Etiological Research Center (CMERC) cohort (2013–2018), CC-MHS provides a rare, high-resolution view of how the COVID-19 pandemic has reshaped the mental health landscape over time.
The study captures a vast array of determinants by integrating physical health indicators—such as Neuro-QoL, fatigue, and cardiac-specific metrics (SAQ-7)—with a rigorous mental health battery encompassing stress (PSS), PTSD (PCL-5), suicidality (SITBI), and impulsivity (BIS). These individual profiles are further contextualized through socioeconomic and environmental lenses, including housing stability, social support (MSPSS), and adverse childhood experiences (ACE), while specifically monitoring COVID-19 related variables such as vaccination impact and the long-term sequelae of Long COVID.
In addition to the baseline survey, eight waves of online mental health surveys were conducted: Wave 1 (Mar 2020), Wave 2 (Aug 2020), Wave 3 (Mar 2021), Wave 4 (Dec 2021), Wave 5 (Nov 2022), Wave 6 (Feb 2024), Wave 7 (Oct 2024), and Wave 8 (Oct 2025).
CC-MHS serves as a critical evidence base for developing targeted public health strategies and clinical interventions. By bridging pre-pandemic cardiovascular-metabolic profiles with contemporary mental health outcomes, this data provides the long-term etiological determinants of well-being in a pandemic-affected world.
Explore the data in PubMed: https://pubmed.ncbi.nlm.nih.gov/40610010/
MeRIT
Mental Health, Resilience, and Immune System in Transplantation Recipients and Donors
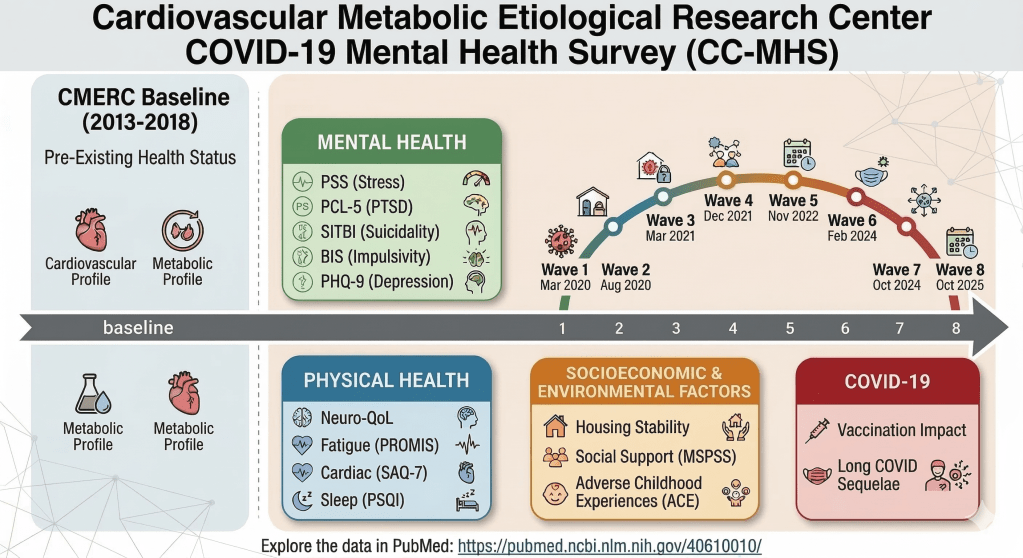
The Mental Health, Resilience, and Immune System in Transplantation Recipients and Donors (MeRIT) cohort is a prospective hospital-based cohort established at Severance Hospital, Seoul, South Korea, to investigate how psychological resilience and mental health influence immune responses and postoperative outcomes among kidney and liver transplant recipients and living donors. MeRIT is distinctive in that it follows both recipients and living donors within a unified longitudinal framework, enabling the study of shared and distinct psychosocial trajectories surrounding transplantation. The cohort captures a broad range of biopsychosocial domains, including mental health, resilience, social support, loneliness, family functioning, sleep, quality of life, cognitive function, autonomic regulation, immune and inflammatory profiles, and transplant-related clinical outcomes. By integrating subjective psychological assessments with objective physiological, biological, and clinical indicators, MeRIT provides a unique platform for identifying modifiable factors that may shape recovery, graft function, complications, and long-term well-being after transplantation.
Data collection began in November 2024 and is conducted across key perioperative stages. Transplant recipients are assessed at hospital admission, discharge, one month post-transplant, and six months post-transplant, while living donors are assessed at admission, discharge, and six months after donation. Questionnaires and interviewer-administered assessments are conducted by trained researchers, and heart rate variability is measured noninvasively during hospitalization as an indicator of autonomic regulation. Blood-based immune and inflammatory markers are obtained using samples collected during routine clinical care, minimizing additional participant burden. In addition, selected physiological and behavioral information may be supplemented through device-based monitoring during hospitalization. Clinical information, including transplantation type, immunosuppressant exposure, graft function, postoperative complications, and long-term outcomes, is systematically extracted from electronic medical records and linked with the cohort data for longitudinal analysis.